Fentanyl
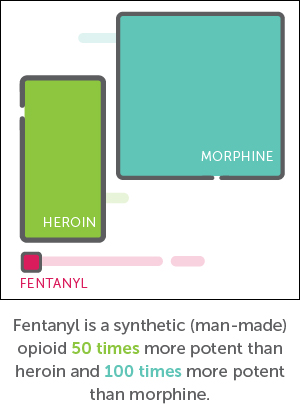
More Americans died from opioid overdoses in 2018 than from traffic accidents or guns. According to the national Centers for Disease Control and Prevention, two-thirds of the almost 47,000 opioid-related deaths were caused by powerful synthetic opioids, primarily fentanyl and its analogs. Sold through illegal drug markets across the U.S., fentanyl is often substituted as a cheaper, if far more dangerous, alternative to heroin and other opioids, like Vicodin and Oxycontin. Fentanyl is also mixed—with or without the user’s knowledge—with street cocaine and other drugs. While the opioid epidemic overall may be leveling off, CDC reports that deaths involving synthetic opioids such as fentanyl climbed 10 percent in 2018. Thus, fentanyl is now driving the most lethal opioid epidemic the U.S. has experienced in the past century.
Drug Strategies convened several meetings in 2018 to identify promising strategies to address the fentanyl crisis. Philip Heymann, Chair of the Drug Strategies Board of Directors, and former U.S. Deputy Attorney General, along with Mathea Falco, President of Drug Strategies, brought together top officials from the U.S. Postal Service, the Department of Justice, FBI, Customs, DEA, FDA, as well as experts from Yale and Harvard Law Schools. After extensive discussions, participants concurred that while federal enforcement and interdiction efforts remain critically important, initiatives at the state level can have immediate impact in reducing fentanyl overdose deaths.
In 2017, just nine states were responsible for nearly 60 percent of all fentanyl related deaths in the U.S. In order to increase public awareness of both the scope of the problem and concrete steps that states have taken to reduce this death toll, Drug Strategies, in collaboration with Shatterproof, developed a report focused on those states that have been most seriously affected. The report offers seven recommendations that should encourage states to take effective action.








Internet Drugs
The Internet, woven into the fabric of our daily lives, has revolutionized everything from communications to commerce. The worldwide web gives us information at the click of a button, including invaluable resources about drug abuse, treatment and prevention. Search engines and social media have influenced how individuals not only seek information or resources, but have also changed the way drug users and dealers find and access both prescription medications and illicit drugs such as fentanyl.
Drug Strategies, an early pioneer in addressing drug policies, treatment, and prevention, was the first to look at the potential impact the internet could have on illegal supplies of opioids. Beginning in 2005, a group of distinguished private business leaders and key government officials convened at the Harvard Law School to develop new strategies to curtail internet drug trafficking to youth. Including Internet regulation, online advertising, payment transfers, delivery services, U.S. and international law, and prevention initiatives. Drug Strategies’ website became a resource for learning more.
Below you will find information about the efforts of Drug Strategies to understand and address the emerging issues of illegal drug sales on the Internet.
- To learn more about the trailblazing 2005 strategy and development of the “Keep Internet Neighbors Safe” Initiative, click here.
- For more about the final recommendations from the “Keep Internet Neighbors Safe” Initiative, click here to read the Policy White Paper.
- For more information on non-medical use of prescription drugs and availability over the internet, click here to read Drug Strategies’ 2005 review of the research literature.
- Click here to read an op-ed from Drug Strategies President Mathea Falco and Harvard Law School Professor Phillip Heymann on this issue published in the Washington Post.
- Click here to read Drug Strategies July 26, 2006 U.S. House Testimony
- Click here to read Drug Strategies May 16, 2007 U.S. Senate Testimony
Treating Teens
A Guide to Adolescent Drug Programs
Working with a team of nationally recognized experts, Drug Strategies prepared a comprehensive assessment of the key elements of effective adolescent drug treatment programs. This guide, the first of its kind, will help parents, teachers, judges, counselors and other concerned adults make better choices about teen treatment options.
Treating Teens…
Identified 9 key elements of effective adolescent drug treatment
Provided a first-of-its-kind online database of current, reliable information on 144 adolescent treatment programs across the country, searchable by state and treatment program
Described in detail 7 promising adolescent programs that included a range of treatment approaches
Provided practical resources, such as hot-line help telephone numbers for each state and questions every parent should ask when considering a program
Ten Important Questions to Ask a Treatment Program
(from Treating Teens)
1. How does your program address the needs of adolescents?
Most treatment programs are designed for adults, not adolescents. Although adolescent treatment capacity has recently begun to expand, relatively few teens can get help for substance abuse in programs that specifically address the unique challenges of adolescence. Experts agree that adolescent treatment cannot just be adult treatment modified for kids. The program should be developmentally appropriate for adolescents. It should also actively engage the family, which is the primary provider of financial support and the dominant force in the adolescent’s life. In addition, the program should address the many different contexts which shape the teen’s environment, such as school, healthcare, recreation, peer groups and where necessary, juvenile court and probation. For residential treatment programs, it is important to know how teens continue their education. Do they attend school in the local community, or does the program include regular onsite classes approved by the local school district with credits that can be transferred to the student’s home school? The nine key elements of effectiveness discussed in Treating Teens provide a framework for assessing how well a treatment program addresses the needs of adolescents.
2. What kind of assessment does the program conduct of the adolescent’s problems?
When a parent or other concerned adult contacts a program—often in response to an immediate crisis—program staff will ask a brief set of screening questions to explore the severity of the youth’s problems and to determine whether a more thorough assessment is required. Screening helps sort out what the teen needs, the severity of the problem, and whether the parent or other referring adult should contact a different kind of program.
Assessment provides a road map for developing an effective treatment plan tailored to the adolescent’s specific needs. Most programs do not use standardized, scientifically-sound screening and assessment instruments. Rather they rely on questionnaires they develop in-house that may have questionable reliability. If the program does not have the necessary services indicated by the assessment, such as intensive psychiatric or medical care, the teen may either be referred to a different program or retained in the original program but sent elsewhere for these services.
3. How often does the program review and update the treatment plan in light of the adolescent’s progress?
The treatment plan, which the program develops after initial comprehensive assessment of the adolescent and his family, provides a guide to recovery that is tailored to the adolescent’s specific needs. These needs will change as the adolescent progresses through the treatment process. Experts suggest that the treatment plan should be reviewed within the first thirty days, and again after sixty and ninety days. In addition, the plan should be reviewed in light of significant developments, such as urinalysis tests that show drug use. As the adolescent nears completion of treatment, the plan should be modified to include continued care and relapse prevention strategies. Follow-up after the teen leaves the program is also important in improving the likelihood that gains made in treatment will not be lost.
4. How is the family involved in the treatment process?
Family involvement in the adolescent’s treatment is critically important for treatment success. Engaging parents—or in the absence of family, the responsible caregiver—increases the likelihood that a teen will stay in treatment and that treatment gains will be sustained after treatment has ended. Programs should encourage parents to participate in counseling, group meetings, drug education and other activities offered by the program. Some programs involve intensive interventions with teens and their families not only at the program, but also at home, school, juvenile facility, probation office and workplace. Occasional telephone calls from program staff to parents are not enough. The more the family is involved, the better the treatment outcomes will be.
5. How do you engage adolescents so that they stay in treatment?
Both the length and the intensity of the treatment vary widely depending on the adolescent’s specific needs. Keeping adolescents in treatment is critically important since completion of treatment is closely related to better outcomes. Retention rates are an important measure of program success. How many clients drop out? How long do they stay in treatment? How many actually complete treatment?
The initial assessment process can engage the teen in treatment by helping him or her to recognize that he or she does have substance abuse and other problems. Motivational interviewing and feedback also help engage the teen, particularly if he or she sees that treatment can address some of the pressing issues in his or her life, including school performance and family relationships. Creative program content targeted to adolescents in terms of examples and developmental appropriateness can make treatment more relevant. The key is to address the everyday concerns of the adolescent so that he or she will be motivated to make the necessary effort to change fundamental behavior patterns.
Practical assistance, such as transportation to the program and other service providers, also helps keep teens in treatment. So, too, do recreational activities, sports events, mentors, after-school tutoring and reward systems, such as vouchers for drug-free urine tests.
6. What are the qualifications of program staff and what kind of clinical supervision is provided?
Qualified staff is critically important to treatment effectiveness. The relationship between the teen and his or her counselor greatly influences the extent to which the program will be able to motivate change and to retain the teen in treatment. In addition to training in substance abuse treatment, staff should be trained to recognize psychiatric problems, understand adolescent development and to work with families. They should also have practical experience in dealing with adolescents and be responsive to the way young people think.
Staff to client ratio is also important: experts suggest that one counselor should treat no more than 20-25 adolescent in outpatient programs, 10-15 clients in intensive outpatient programs, and 4-8 clients in residential programs. In addition, programs should provide regular clinical supervision several times a week by more experienced staff to provide guidance for counselors as well as to monitor progress in staff-client interactions.
7. Does the program offer separate single sex groups as well as male and female counselors for girls and boys?
Recent research points to significant differences between male and female adolescent drug users. Girls with drug abuse problems are more likely to have serious mental health problems, particularly depression, anxiety and post-traumatic stress disorder. They are also more likely to be the victims of sexual and physical abuse, often by family members or older friends. Boys more often have conduct disorders, including aggressive, disruptive and even violent behavior, and they, too, may have been victims of sexual abuse.
Single sex group sessions provide the opportunity to focus on issues that might be difficult to discuss in co-ed groups. Teenage girls often strive for approval from males rather than focusing on their own problems. In addition, they may be reluctant to talk freely in front of males about their experiences, which many regard as shameful. Working with women counselors and with other girls in group therapy provides girls with a psychological safe haven to explore problems related to their substance abuse. Boys, too, can benefit from single sex group focus on disruptive behaviors, date rape, HIV risks, and understanding the responsibilities of becoming an adult. They can also learn new behaviors and attitudes from male counselors who provide positive role models.
8. How does the program follow up with the adolescent and provide continuing care after treatment is completed?
The period following treatment is vitally important in consolidating the gains made in treatment. Most adolescents relapse in the first three months after treatment. However, effective continuing care services substantially increase the teen’s chances of successful, sustained recovery. These services include relapse prevention training, follow-up plans and referrals to community resources. In addition, the program should schedule periodic check-ups with the adolescent at one month, three months and one year after completing treatment. Wherever possible, more frequent contact is preferable; both to monitor the teen’s progress and to make sure the teens and his or her family are receiving the necessary services in the community.
Most programs provide referrals to community resources, including Twelve Step meetings and group therapy, where available. Some programs offer continuing services, such as counseling and education, after the period of formal treatment is completed. Less frequently, programs develop a comprehensive continuing care plan while the teen is still in treatment so that the transition back into the community is as seamless as possible.
9. What evidence do you have that your program is effective?>
Very few programs have formal, scientific outcome evaluations that measure treatment success. However, in the absence of such evaluations, other information can shed light on the effectiveness of a program. For example, completing treatment is closely related to positive outcomes.>
Retention rate is an important indicator of effectiveness. How many teens drop out? How long do they stay? How many actually complete treatment? Even without formal evaluations, programs should be able to provide accurate information on client retention and completion. Programs should also be able to demonstrate how they measure the individual teen’s progress through treatment. Does the program routinely report on key indicators of behavioral change? Do urine tests come back clean? Is school performance improving? Is aggressive behavior diminishing? Are family relationships getting stronger? In short, can the program show that the trajectory of the teen’s life has changed for the better?
10. What is the cost of the program?
The cost of drug treatment programs varies widely, depending on the program, its location and the type of care offered. Residential programs are generally the most expensive option, since they provide live-in facilities and around the clock supervision by trained counselors. For example, the rates charged by three of the programs described in this guide, Chestnut Health, Hazelden and Thunder Road, range from $500 to over $800 per day. Outpatient treatment is much less expensive, since the adolescent lives at home. For example, MDFT (Multidimensional Family Therapy), an outpatient program which is described in this guide, costs $164 per week. An intensive version of MDFT is more expensive ($384 per week) because of the additional services provided.
Health plans have not generally offered full coverage for substance abuse treatment, though recently enacted federal legislation requires group health insurance plans that cover addiction and/or mental illness to provide these benefits on par with benefits provided for other illnesses; while the law does not require insurance plans to offer addiction or mental health treatment, it does restrict group health insurance plans from setting higher co-payments or deductibles for these services in comparison to those charged for medical or surgical services.
Medicaid coverage for substance abuse treatment varies by state. Some states provide Medicaid coverage for a full range of treatment options, while others cover only inpatient detoxification. The recently passed Patient Protection and Affordable Care Act expands eligibility for Medicaid coverage and requires that newly eligible Medicaid recipients receive substance abuse and mental health services on par with medical services. For adolescents under the jurisdiction of the juvenile justice system, costs for participation in certain treatment programs are covered by the juvenile justice system.
Interactive Tools
Bubblemonkey
Developed by Drug Strategies, bubblemonkey.com was a groundbreaking interactive website that provided youth with accurate, anonymous information on drugs, substance abuse, and treatment. As an accessible, educational resource, bubblemonkey.com gave adolescents a place to ask questions and safely learn about drugs and alcohol. (BubbleMonkey was previously available in Spanish as well.)
Check out URLWire’s report on bubblemonkey.com: BubbleMonkey.com Web Site Teaches Teens About Drugs, Alcohol.
Tunnel Tail



